
You may know that colon polyps can lead to colon cancer, but you may not know what causes colon polyps. The answers may surprise you.
Colon polyps are small clumps of cells that can form on the lining of the lower intestine or colon. Polyps can occur in several locations throughout your gastrointestinal tract, but they most commonly occur in your colon. Polyps can also develop in the last part of the colon, known as the rectum. Doctors often refer to conditions occurring in the colon and rectum together, using the term “colorectal.”
Polyps often look like bumps growing from the inside lining of your intestine and protruding outward into your colon. Some polyps grow on a “stalk,” which makes them look like mushrooms. The stalk allows these polyps to “flop” around inside the intestine. Other polyps can have a wide base, so they lie flat against the colon. Polyps vary in size, ranging from less than one-quarter of an inch to several inches in diameter. They can be scattered throughout the colon, which is about 5 feet long.
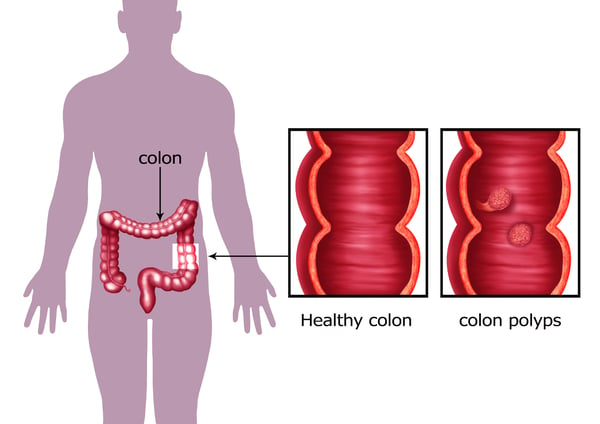
Most polyps do not cause symptoms, although larger colon polyps can cause blood in the stool. While most colon polyps are harmless, some can develop into colon cancer. You can reduce your risk of developing colon cancer by sticking to the recommended colorectal cancer screening schedule and by having polyps removed.
Learn about how colorectal cancers are detected and diagnosed.
Types of Colon Polyps and Their Causes
Abnormal cell growth also referred to as a neoplastic disease, is what allows both cancerous (malignant) and non-cancerous (benign) tumors to grow. There are two main types of polyps: non-neoplastic and neoplastic. Non-neoplastic polyps do not usually become cancerous; neoplastic polyps can become cancerous.
Non-Neoplastic Polyps
There are several types of non-neoplastic polyps that are not likely to become cancerous. These non-neoplastic polyps include inflammatory polyps, hyperplastic polyps, and hamartomatous polyps.
- Inflammatory polyps often occur in people with inflammatory bowel disease (IBD).
- A hyperplastic polyp is a growth of extra cells that project out from tissue; they often develop where the body has repaired damaged tissue.
- Hamartomatous polyps contain a mixture of tissue cells; they can occur as the result of faulty development and are rare in adults but are the most common types of polyps in children.
Neoplastic Polyps
There are also several types of neoplastic polyps, which may become cancerous. These polyps include adenomas and serrated polyps.
- To the naked eye, adenomas in the colon look similar to healthy cells lining the colon – these cells look quite different under the microscope, however.
- Serrated polyps look quite different from healthy colon cells; serrated polyps stick out from the surface of the colon. Serrated polyps have a saw-toothed appearance under the microscope.
The larger the polyp, the greater the risk it has of becoming cancerous. This is particularly true with neoplastic polyps.
Factors that Increase Your Risk of Developing Colon Polyps
Medical researchers have not yet established the exact cause of colon polyps in all cases, but they have determined that certain factors can increase your risk of developing colon polyps. You can control some of these risk factors, such as diet and exercise, but cannot control others.
Aging
Colon polyps are uncommon in people in their 20s, according to the American Society for Gastrointestinal Endoscopy (ASGE), but more than 40% of people in their 50s have precancerous colon polyps. In fact, the ASGE says that being over the age of 50 is the biggest risk factor for developing colon polyps.
Your doctor may recommend starting colorectal cancer testing if you are age 50 or older and have an average risk of developing cancer affecting the colon or rectum.
Family History of Polyps or Colon Cancer
You may be at higher risk of developing colon polyps if someone in your family has had polyps or colon cancer. This is especially true if you have a first-degree relative, such as a parent or sibling, with colon polyps or colon cancer, but it is also true if you have a grandparent, an aunt, or an uncle with those conditions.
Your Personal Medical History
You may be at higher risk of developing colon polyps if you have inflammatory bowel diseases, such as Crohn’s disease or ulcerative colitis. These conditions cause inflammation of the colon, a condition known as colitis. Research published in BMC Gastroenterology shows that some types of polyps are more common in patients with IBD than in those without the condition, and the research shows that the polyps developed in the part of the colon affected by colitis.
Other research published in the Polish Journal of Surgery shows colon polyps are more common in people with diabetes; this could be because of certain medications patients take to control their blood sugar.
A publication in the Annals of Clinical & Laboratory Science shows polyps are more common in people with diabetes or chronic kidney disease.
The Foods You Eat
Your body can have trouble digesting certain foods in ways that lead to the development of colon polyps. Bile and digestive juices may have trouble processing fatty foods. For example, byproducts of these foods can become lodged in the colon and lead to the growth of polyps there.
Specifically, eating foods high in saturated fat, red meat such as beef and pork, and processed meat, including lunchmeat, bacon, sausage, and hot dogs, can support the development of colon polyps.
Certain Lifestyle Choices
Research suggests that people who drink alcohol have a higher risk of developing colon polyps; other research suggests a link between cigarette smoking and colon polyps.
Being Overweight
A 2012 review of past studies also links obesity with the development of colon polyps. It found that 22% of overweight and obese participants had colon polyps, and 19% of participants of normal weight had polyps in their colon.
It also showed that the risk of polyps grew with increasing body mass index (BMI), a common measure of body fat that helps doctors determine if a patient is overweight or obese.
Related blog: What Are Colorectal Cancer Risk Factors, and Who Is at Risk?
Prevention of Cancer from Colon Polyps
While it is not always possible to prevent polyps from developing in the colon, your doctor can remove polyps before the harmless bumps turn into cancer. Doctors can detect and remove colon polyps with a procedure known as a colonoscopy, in which they insert a flexible tube through the anus and into the colon. A camera attached to the thin tube allows your doctor to see the polyps along the entire colon.
Tiny tools, such as wire loops or forceps, attached to the colonoscopy tube, let your doctor remove suspicious polyps. Your doctor can also use a colonoscopy to take small tissue samples, known as biopsies, to send to the laboratory for analysis. Because the lining of the bowel is not sensitive to cutting, polyp removal does not hurt.
Colorectal cancer specialists can also perform a sigmoidoscopy, which only looks at the lower part of the colon and the rectum. Other techniques for detecting colon polyps involve testing stool specimens for traces of blood. Compared to a colonoscopy, at-home colon cancer tests offer much more convenience, and while you can’t solely use at-home tests for colorectal cancer screening throughout your life, you might be able to use this option first.
Watch to see a comparison of at-home colorectal cancer test kits versus a colonoscopy.
Unlike colonoscopy, these tests do not give doctors the opportunity to remove the polyps, which is why your doctor will likely recommend colonoscopy over other types of screening tests. Read our blog to learn more about options: Screening at Home: What You Need to Know About Colon Cancer Testing.
To learn more information about colon polyps, their causes, prevention, and treatment, consult with your doctor or colon cancer specialist.

